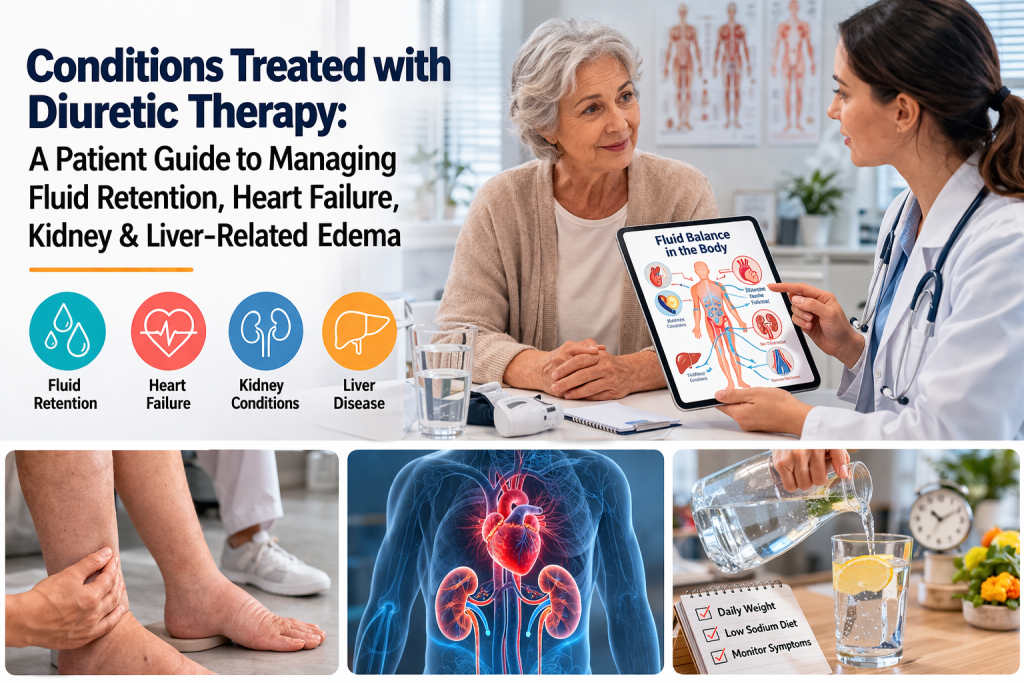
Swelling in the legs, a tight abdomen, sudden weight gain, or shortness of breath can look like separate problems at first. In practice, they often point to one core issue: the body is holding on to more fluid than it can comfortably manage. That extra fluid does not appear out of nowhere. It usually reflects a larger disease process involving the heart, liver, or kidneys. A diuretic such as furosemide may help move some of that fluid out of the body, but the bigger clinical question is always the same: what is driving the overload in the first place?
This article focuses on the conditions behind fluid retention rather than on the medication itself. That distinction matters. A loop diuretic can reduce congestion, ease breathing, and lower swelling, but it does not cure heart failure, reverse cirrhosis, or heal damaged kidneys. When the underlying disease is missed, people may briefly feel better while the real problem continues to progress. For patients, caregivers, and health content readers, understanding the disease state behind the symptom pattern is often the most useful first step.
In current clinical practice, furosemide is commonly used when edema is linked to congestive heart failure, cirrhosis, or renal disease, including nephrotic syndrome. It may also be used in some adults with hypertension, although fluid-overload states are the more clinically important focus for most patient education. The practical takeaway is simple: swelling is not a diagnosis. It is a signal. The cause of that signal determines the urgency, the workup, and the long-term treatment plan.
Key takeaways
- Fluid retention is often a symptom of heart failure, cirrhosis with ascites, chronic kidney disease, or nephrotic syndrome.
- Shortness of breath with fluid overload may mean pulmonary congestion or pulmonary edema, which can become an emergency.
- Diuretics can relieve symptoms, but they work best when paired with treatment of the underlying condition and close monitoring of kidney function, electrolytes, blood pressure, and weight.
- Rapid swelling, chest symptoms, severe breathlessness, confusion, or reduced urination should never be treated as a minor issue.
What fluid overload really means
The body normally keeps a careful balance between the fluid inside blood vessels, the fluid between tissues, and the fluid filtered by the kidneys. That balance depends on circulation, kidney filtration, hormonal signals, sodium handling, and blood proteins such as albumin. When one or more of those systems breaks down, fluid can move into tissues or body cavities. That is why a person may notice ankle swelling, facial puffiness, abdominal distension, or a heavier feeling in the chest.
Clinicians often use the term edema for swelling caused by excess fluid in tissues. The swelling may be localized or widespread. In advanced disease, it may come with fast weight gain, tighter shoes, rings that no longer fit, or difficulty sleeping flat. In people with liver disease, fluid may collect in the abdomen and create ascites. In people with heart disease, fluid may back up into the lungs and make breathing harder. In kidney disorders, sodium and water retention may build gradually until swelling becomes impossible to ignore.
Not all swelling is dangerous, but the pattern matters. Swelling in both legs with breathlessness raises different concerns than swelling in one calf after a long flight. Likewise, a firm distended abdomen in cirrhosis is different from mild evening ankle swelling in hot weather. Good patient education should make this clear: the symptom may look simple, but the physiology behind it is often complex.
Heart failure: when the pump falls behind
Heart failure is one of the most common reasons adults develop clinically significant fluid retention. Despite the name, it does not mean the heart has stopped. It means the heart is no longer pumping well enough to meet the body’s needs, either because it cannot squeeze effectively, cannot relax and fill properly, or both. As the pumping problem worsens, pressure rises in the circulation, the kidneys interpret that reduced forward flow as a signal to hold on to salt and water, and fluid begins to accumulate.
That process explains why heart failure often presents with two sets of symptoms at the same time. One group reflects poor forward circulation: fatigue, lower exercise tolerance, weakness, brain fog, and reduced stamina. The other reflects congestion: swelling in the feet and legs, weight gain, abdominal fullness, frequent nighttime urination, cough, and shortness of breath. Some patients first notice that they need extra pillows to sleep, while others become winded doing basic tasks such as dressing or walking across a room.
Heart failure can affect the left side of the heart, the right side, or both. Left-sided failure is more strongly linked to fluid backing up toward the lungs, so people often feel breathless, especially when lying flat. Right-sided failure is more strongly linked to peripheral swelling, neck vein fullness, and abdominal congestion. In real-world patients, the picture is often mixed. That is why the condition can look so different from one person to the next.
The common causes of heart failure include coronary artery disease, prior heart attack, long-standing high blood pressure, cardiomyopathy, valve disease, and certain rhythm problems. Obesity, diabetes, sleep apnea, kidney disease, and aging can all increase risk or complicate management. Importantly, fluid retention in heart failure is not just a cosmetic issue. It often signals worsening hemodynamics and a higher risk of hospitalization if the trend continues unchecked.
Diagnosis usually combines the story, the physical exam, lab tests, and imaging. Clinicians may look for weight gain, crackles in the lungs, edema, elevated jugular venous pressure, or liver congestion. Blood tests such as BNP or NT-proBNP can help, and echocardiography remains central because it shows how well the heart fills and pumps. The treatment plan then depends on the heart failure type, severity, and what is driving it.
Where does Lasix fit here? Mainly as a decongestive tool. It helps remove excess fluid so breathing improves and swelling goes down. That symptomatic relief can be dramatic, but it is only one part of treatment. Modern heart failure care also focuses on disease-modifying therapy, sodium awareness, blood pressure control, rhythm management when needed, and close follow-up when symptoms change. In other words, the water pill may make the patient feel better quickly, but the rest of the treatment plan is what influences longer-term outcomes.
Cirrhosis and ascites: when portal pressure and low effective circulation change the rules
Cirrhosis is severe scarring of the liver that disrupts normal blood flow through the organ and interferes with its metabolic functions. Many people think of cirrhosis only as a liver problem, but its consequences are systemic. As scarring advances, pressure builds inside the portal venous system, a problem called portal hypertension. At the same time, the body develops circulatory changes that make the kidneys retain sodium and water. The result is a classic pattern: ascites in the abdomen, edema in the legs, and sometimes pleural fluid around the lungs.
Ascites is often the first major sign that cirrhosis has become decompensated. Patients may describe a growing belly despite poor appetite, early fullness when eating, shortness of breath from abdominal pressure, or a steady need to loosen clothing. Lower-extremity swelling is also common. Because cirrhosis changes albumin production and blood vessel tone, fluid shifts out of the bloodstream more easily, making the swelling problem harder to control than many people expect.
This is the reason liver-related fluid retention cannot be treated like ordinary bloating. Ascites signals clinically significant liver disease and deserves formal medical evaluation. New or worsening ascites may lead to diagnostic paracentesis, assessment for infection, medication review, sodium restriction counseling, and a discussion about transplant evaluation in appropriate patients. It also raises the risk of complications such as spontaneous bacterial peritonitis, kidney injury, electrolyte problems, and recurrent hospitalizations.
Diuretics are commonly used in cirrhotic ascites, but the setting requires caution. If fluid is mobilized too aggressively, kidney function can worsen, sodium can fall, and encephalopathy risk can increase in vulnerable patients. That is why outpatient liver care often relies on a structured plan rather than a casual “take a water pill” approach. Weight trends, abdominal girth, creatinine, sodium, potassium, and symptoms all matter. In some patients, large-volume paracentesis becomes necessary because medication alone is not enough.
Kidney disease and nephrotic syndrome: when filtration fails or protein leaks
The kidneys do far more than make urine. They filter waste, regulate electrolytes, help control blood pressure, and fine-tune how much sodium and water the body keeps. When kidney function declines, fluid regulation becomes less reliable. In advanced chronic kidney disease, the kidneys may struggle to remove excess salt and water, and edema becomes more likely. Patients may notice swelling in the legs, feet, or ankles, sometimes paired with fatigue, loss of appetite, nausea, or changes in urination.
One especially important fluid-retention pattern appears in nephrotic syndrome. This is not one disease but a syndrome caused by abnormal leakage of protein through the kidney’s filters. The major features include heavy protein loss in the urine, low albumin in the blood, swelling, and abnormal lipid levels. Puffiness around the eyes, lower-extremity edema, abdominal swelling, and rapid weight gain are common clues. Because albumin helps keep fluid inside the bloodstream, low albumin makes it easier for fluid to move into tissues.
Nephrotic syndrome can result from kidney-limited diseases such as focal segmental glomerulosclerosis, membranous nephropathy, or minimal change disease, but it can also be linked to systemic conditions such as diabetes, lupus, amyloidosis, or infections. That is why the presence of edema in nephrotic syndrome is only one piece of the workup. The real task is identifying what is damaging the glomeruli and how far the disease has progressed.
Diuretics may help reduce swelling in kidney disease and nephrotic syndrome, but response is sometimes less predictable than expected. In nephrotic states with marked hypoproteinemia, the diuretic effect may be blunted, and adverse effects may become more likely. That is one reason kidney-related edema often requires more than a prescription alone. Sodium intake, blood pressure control, urine protein assessment, kidney function monitoring, and disease-specific treatment all shape the outcome.
The broader lesson is that kidney-related swelling is not just “water weight.” It may reflect progressive CKD, significant protein loss, or both. When accompanied by foamy urine, reduced urine output, uncontrolled blood pressure, or fatigue, it deserves careful evaluation rather than self-treatment.
Acute pulmonary edema: the emergency face of fluid overload
Some forms of fluid overload become emergencies quickly, and acute pulmonary edema is one of the clearest examples. In this scenario, fluid collects in the lungs and interferes with gas exchange. Patients may feel as though they cannot get enough air, especially when lying flat. They may cough, breathe rapidly, panic, speak only in short phrases, or produce frothy sputum. This is not a “watch and wait” situation.
Acute pulmonary edema is often related to severe decompensated heart failure, but it can also appear with severe hypertension, major cardiac events, kidney failure, toxic inhalation, or other critical illnesses. Because breathing is immediately affected, emergency assessment focuses on oxygenation, circulation, imaging, and rapid treatment of the underlying trigger. In hospital settings, loop diuretics may be part of treatment, but they are only one component of a broader emergency response.
For educational content, this section matters because many readers underestimate the link between swelling and breathing danger. A person who has gained several pounds of fluid, cannot lie flat, and suddenly becomes very short of breath may not just be “retaining water.” They may be developing life-threatening lung congestion.
How clinicians figure out what is causing the swelling
Because edema has many causes, the best workup starts with pattern recognition. Bilateral leg edema with orthopnea points clinicians toward heart failure. A distended abdomen with liver disease history points toward ascites. Puffy eyelids, foamy urine, and low albumin raise suspicion for nephrotic syndrome. Medication induced edema, venous insufficiency, lymphatic disorders, thyroid disease, pregnancy-related swelling, and blood clots also stay on the differential depending on the story.
History matters. Clinicians usually ask when swelling started, whether it is symmetric, whether breathing changed, how much weight was gained, what the sodium intake looks like, and whether urine output has changed. They also review alcohol use, liver disease history, heart disease, diabetes, hypertension, autoimmune conditions, and current medications. Physical examination adds more detail by looking for pitting edema, lung crackles, abdominal fluid, jugular venous distension, skin changes, and signs of poor circulation.
Testing is guided by suspicion. Kidney panels, liver tests, albumin, natriuretic peptides, urine protein assessment, chest imaging, abdominal ultrasound, and echocardiography may all be relevant. The goal is not simply to confirm that fluid is present. It is to identify why the body is holding on to it and how dangerous the overall condition has become.
Where loop diuretics fit into treatment
Furosemide belongs to the loop diuretic class and is used because it can move sodium and water out of the body more powerfully than many milder diuretics. In practical terms, that makes it useful for clinically meaningful edema, not just minor puffiness. According to FDA labeling, it is indicated for edema associated with congestive heart failure, cirrhosis of the liver, and renal disease, including nephrotic syndrome, and it can also be used in adults with hypertension.
That said, the medication has limits. It can reduce congestion, but it can also cause dehydration, low blood pressure, worsening kidney function, low potassium, low sodium, low magnesium, and other electrolyte problems if not monitored carefully. In cirrhosis, aggressive fluid removal can destabilize the patient. In nephrotic syndrome, low protein states may reduce effectiveness. In older adults, the balance between symptom relief and adverse effects can shift quickly. The need for monitoring is not a technical footnote. It is central to safe use.
For readers, the right mindset is this: diuretics treat the fluid consequence of disease, not the disease itself. A patient whose swelling improves still needs to know whether the driver is heart failure progression, worsening liver reserve, kidney damage, or another process entirely.
Daily habits that influence symptom control
Although the root disease guides treatment, everyday habits still matter. Sodium intake plays a major role in fluid retention. In both heart failure and cirrhotic ascites, a high-salt diet can make swelling harder to control and can undermine the benefit of prescribed medicines. Daily weights are also useful because they can reveal fluid trends before symptoms become dramatic. A sudden jump on the scale may be more informative than appearance alone.

Medication review is equally important. Nonsteroidal anti-inflammatory drugs can worsen kidney perfusion and make diuretics less effective. Some over-the-counter cold products can raise blood pressure. Missed doses of cardiac medications or liver-related therapies may indirectly worsen congestion. Readers should also understand that “drinking less water” is not a universal fix. Fluid restriction is condition-specific and should follow clinical guidance, not guesswork.
Follow-up matters because fluid disorders change. Lab work, blood pressure, renal function, electrolytes, and symptom trends help clinicians adjust therapy before a small imbalance becomes a hospitalization. That is especially true after a recent medication change, a heart failure flare, a new ascites diagnosis, or a kidney disease exacerbation.
When swelling is caused by something else
Even though heart, liver, and kidney disorders are major causes of edema, they are not the only ones. Chronic venous insufficiency can cause dependent leg swelling. Certain blood pressure medicines can trigger ankle edema. Lymphedema behaves differently from pitting fluid overload. Deep vein thrombosis may cause one-sided swelling, pain, or redness. Pregnancy, infections, severe malnutrition, and endocrine disorders also belong on the broader list.
That is why responsible medical content should avoid oversimplifying all swelling as a fluid problem fixable with a single pill. The appearance of edema can be similar across very different diseases. The pattern, associated symptoms, and test results are what separate a chronic outpatient issue from an emergency or a disease that needs a completely different treatment path.
Conclusion
When a patient develops edema, the real story usually starts deeper than the swelling itself. Heart failure causes congestion because the circulation cannot keep up. Cirrhosis causes ascites and edema because portal pressure and systemic changes alter fluid balance. Kidney disease and nephrotic syndrome do it because filtration and protein handling break down. Lasix can be valuable in each setting, but only as part of a larger disease based plan.
That is the most useful frame for readers and patients alike: do not ask only how to dry out the fluid. Ask why the fluid appeared, what system is failing, and what warning signs suggest the condition is becoming more dangerous. Good treatment starts when the symptom is connected back to the disease that created it.
References and editorial sources
- FDA prescribing information for LASIX (furosemide) tablets, reviewed for labeled uses and major safety warnings.
- NHLBI heart failure educational pages, reviewed for symptom patterns, causes, and treatment framing.
- NIDDK materials on cirrhosis, chronic kidney disease, nephrotic syndrome, and glomerular disease, reviewed for disease descriptions and edema mechanisms.
- MedlinePlus pulmonary edema reference, reviewed for emergency warning signs and presentation.
- AASLD ascites guidance and educational materials, reviewed for cirrhosis-related fluid retention context.
Editorial note: This article is educational content for a general audience and is not a substitute for personalized medical care.
FAQ
Can swelling be the first sign of heart failure?
Yes. Some people first notice ankle swelling, weight gain, or shortness of breath before they ever hear the words heart failure. In others, fatigue and reduced exercise tolerance show up first. Swelling becomes more concerning when it is paired with breathlessness, trouble lying flat, or a rapid increase in body weight.
Why does liver disease cause belly swelling?
Cirrhosis disrupts blood flow through the liver and changes how the body handles fluid and sodium. This can lead to portal hypertension and fluid accumulation in the abdominal cavity, called ascites. The issue is not simple bloating; it reflects advanced liver-related circulatory changes.
Is all kidney-related swelling a sign of kidney failure?
No. Swelling can occur in several kidney disorders, including nephrotic syndrome and advanced chronic kidney disease. The key question is what type of kidney problem is present, whether protein is leaking into the urine, and how much kidney function is left.
Does a diuretic cure the underlying disease?
No. It can reduce congestion and improve symptoms, but the heart, liver, or kidney condition still needs its own evaluation and treatment plan. Symptom relief is important, but it is not the same as disease reversal.
When is swelling an emergency?
It becomes urgent when it comes with chest pain, severe shortness of breath, confusion, fainting, very low urine output, one-sided painful leg swelling, coughing up frothy sputum, or rapid deterioration. Those features can signal pulmonary edema, blood clot, severe heart failure, or acute kidney problems.
Why are blood tests and weight checks so important during treatment?
Because the same medicines that reduce fluid can also change kidney function and electrolytes. Daily weights help detect fluid shifts early, while blood tests help clinicians balance symptom control with safety.
What stood out to me here is the reminder that swelling is only the visible part of the problem.
A lot of people assume leg edema is just a circulation issue or too much salt, but this article
does a good job showing how the heart, liver, and kidneys each create fluid overload in different ways.
That distinction really matters because the right treatment depends on the real cause.
The section on heart failure was especially useful. Many readers know about shortness of breath, but fewer people connect it with rapid weight gain, abdominal fullness, or needing more pillows at night. That combination of symptoms makes the explanation feel practical instead of overly textbook. It is the kind of information caregivers can actually use.
Bilateral leg edema combined with orthopnea suggests heart failure. A history of abdominal distension in the presence of liver disease suggests ascites.
Depending on the patient’s medical history, the differential diagnosis also includes medication-induced edema, venous insufficiency, lymphatic disorders, thyroid disease, pregnancy-related edema, and blood clots. Wish you all the best.